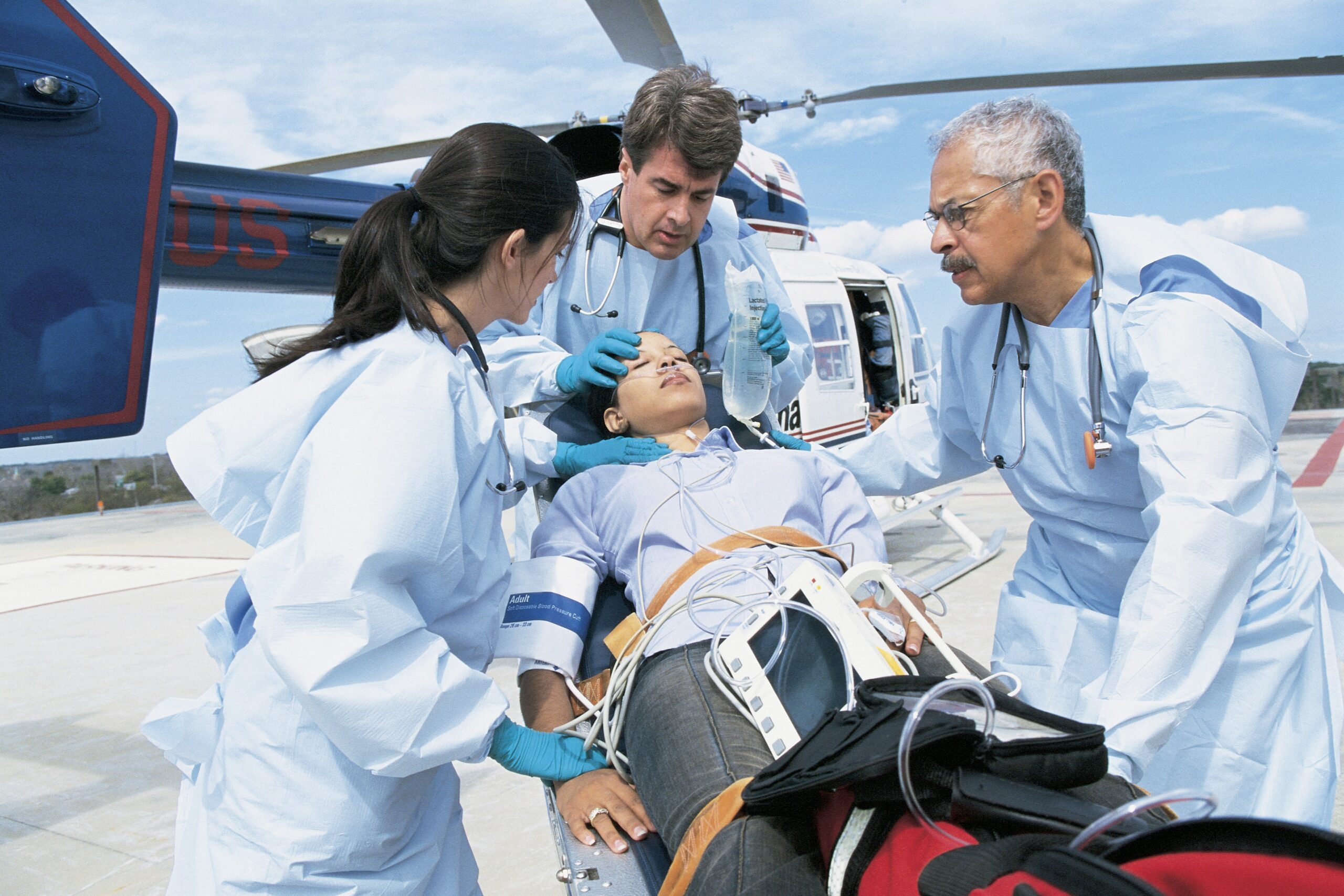
Emergency medicine plays a vital role in modern healthcare. Every day, emergency departments treat critical injuries, sudden illnesses, and life-threatening conditions. Over the past decade, the field has evolved quickly. New technology, smarter triage systems, and improved training help doctors respond faster and save more lives. At the same time, emergency departments face rising patient numbers, staffing shortages, and complex medical cases. Because of these pressures, healthcare leaders continue to search for better solutions. As a result, emergency medicine today reflects a mix of innovation, challenges, and remarkable progress that is reshaping how hospitals deliver urgent care.
Technological Advances Transform Emergency Medicine
Technology now drives many improvements in emergency medicine. For example, artificial intelligence tools help doctors read medical scans within seconds. These systems detect strokes, internal bleeding, and fractures faster than traditional workflows. As a result, physicians can start treatment sooner. Telemedicine also allows specialists to assist emergency doctors remotely. When a hospital lacks a neurologist or trauma surgeon, a remote expert can guide the medical team through critical decisions.
In addition, portable diagnostic tools improve care directly at the bedside. Handheld ultrasound devices help physicians check internal injuries without moving unstable patients. Meanwhile, advanced patient monitoring systems continuously track heart rate, oxygen levels, and blood pressure. Because these systems send alerts immediately, clinicians can act before a patient’s condition worsens. Consequently, technology strengthens the speed and precision of emergency medicine.
Modern Triage Systems Improve Patient Flow
Efficient triage remains the backbone of emergency medicine. When patients arrive at an emergency department, medical staff must quickly decide who needs immediate treatment. Modern triage systems now rely on digital tools and predictive analytics. These tools analyze symptoms, vital signs, and patient history within seconds. Therefore, doctors can prioritize the most urgent cases while still carefully monitoring the others.
Furthermore, hospitals now redesign emergency departments to reduce delays. Fast-track units treat patients with minor injuries or illnesses, which keeps critical care areas open for severe cases. At the same time, digital patient-tracking boards display real-time updates across the department. As a result, nurses, doctors, and support staff coordinate care more effectively. This improved workflow helps emergency medicine teams treat more patients without sacrificing quality.
Rising Patient Demand Creates New Challenges
Despite progress, emergency medicine continues to face growing pressure. Emergency departments across the United States report record patient visits each year. Several factors drive this trend. Many people lack access to primary care, so they seek treatment in emergency rooms instead. Additionally, an aging population brings more complex medical conditions that require urgent attention.
Long wait times often follow this surge in demand. When emergency departments operate beyond capacity, staff must work under extreme pressure. Moreover, overcrowding increases the risk of delayed diagnoses or treatment errors. To address this issue, hospitals invest in community health programs and urgent care partnerships. These strategies help redirect non-critical cases while preserving emergency medicine resources for true emergencies.
Staffing Shortages Affect Emergency Departments
Healthcare staffing shortages now challenge emergency medicine across the country. Many hospitals struggle to recruit and retain experienced emergency physicians and nurses. The work environment often involves long shifts, high stress, and emotional strain. As a result, burnout rates remain high among emergency medical professionals.
However, healthcare systems actively explore solutions. Many hospitals now expand residency programs to train more emergency physicians. Additionally, new team-based care models distribute responsibilities across physicians, nurse practitioners, physician assistants, and paramedics. Because these teams share the workload, patient care improves while staff stress decreases. Over time, these strategies may strengthen the emergency medicine workforce.
Training and Simulation Strengthen Medical Skills
Training programs in emergency medicine now rely heavily on simulation technology. Modern medical simulation labs recreate real emergency scenarios such as cardiac arrest, trauma injuries, and severe infections. During these exercises, medical teams practice quick decision-making and coordinated care. Consequently, clinicians build confidence before they face real emergencies.
Moreover, simulation allows teams to review mistakes safely. After each training session, instructors analyze decisions and identify ways to improve. Because emergency medicine often requires split-second judgments, repeated practice proves essential. In addition, virtual reality training now introduces immersive patient scenarios that improve diagnostic thinking. These innovations ensure that emergency medicine professionals remain prepared for complex situations.
Community Partnerships Support Emergency Medicine
Emergency medicine works best when hospitals collaborate with community healthcare providers. Many hospitals partner with urgent care centers, mental health clinics, and primary care providers to reduce unnecessary emergency visits. When patients receive proper preventive care, they often avoid emergencies entirely.
At the same time, public health campaigns educate communities about emergency symptoms such as stroke or heart attack. Quick recognition can save lives because early treatment often prevents severe complications. Furthermore, emergency medical services coordinate closely with hospital teams during patient transport. This communication allows doctors to prepare treatment before the patient arrives, thereby speeding lifesaving care.
The Future of Emergency Medicine
The future of emergency medicine will likely include even greater technological integration. Artificial intelligence may soon assist with diagnosis, treatment planning, and patient monitoring. Meanwhile, wearable health devices could send real-time health alerts directly to emergency departments. These developments allow doctors to intervene before a crisis occurs.
Nevertheless, innovation alone cannot solve every challenge. Healthcare systems must also address staffing shortages, hospital capacity, and equitable access to care. Strong leadership and smart policy decisions will shape the next phase of emergency medicine. With continued investment and collaboration, the field will continue to evolve while maintaining its central mission: saving lives when every second matters.